Love Island vibes, the kindness of nurses and the magic of the NHS
Why my 10-day hospital stay is an experience I'll never forget
If you’ve never had major surgery, you may imagine recovery the way I did until two weeks ago. I thought you went under the knife, then spent the next week or so in a hospital bed, mostly horizontal, either sleeping or working your way through a pile of books and TV shows. I had prepared for my operation to remove my sternum by carefully curating my recovery reading and downloading season two of The White Lotus.
But in the week after my surgery, I couldn’t read or watch a thing. It was more like an intensive survival boot camp than the sleepy recovery I had imagined. It was both the hardest and one of the most beautiful weeks of my life, where I was treated by nurses I will remember forever, and made some incredibly special friendships.
They say you forget the pain of childbirth, and I already feel like I’ve forgotten the worst bits of the aftermath of my surgery, which I repeatedly described as ‘hideous’. But my 10 days at the Royal Brompton hospital in west London felt really profound, so I want to share as much of it as I can before I forget.
If you’re new to this newsletter, you can read about my secondary breast cancer and the reasons for my surgery here:
How it started
Two days before my long-planned surgery, my partner's beloved father died suddenly. Pete had been living with Parkinson's disease for well over a decade, but he caught pneumonia suddenly and didn't survive. We had seen him two weeks earlier, smiling and joking on New Year’s Day. I had only known him for a year and a half, but I felt like we had a special relationship, communicated through cheeky grins and witty asides. I knew how happy he was that his son had found me.
Mark was devastated, and I wanted nothing more than to be by his side, but I knew I had to focus on my own surgery and recovery. So as he travelled south to say goodbye to his father and to be with his mum, I stayed home alone. Mark was no longer able to take me to the hospital, and the next time I saw him was when I woke up from the anaesthetic.
The night before I was due to go into hospital, I had a fever of 38.9°C. After a few frantic calls to the Macmillan hotline, we concluded the fever was down to the iron infusion I’d been given a few days earlier to increase my red blood cells in preparation for the surgery. I was told to take paracetamol and get some sleep.
I woke the next morning with a horrible migraine. I no longer had a temperature, but I vomited before breakfast and felt sure I wouldn’t be allowed the surgery I’d been waiting months for. Then suddenly, I felt fine. I knew I’d had a migraine from the stress of it all. I talked to my nurse at the Royal Marsden and also called the Royal Brompton. A few hours later, a close friend drove me to the hospital.
Pre-surgery, I’d had every preparation under the sun: PET-CT and CT scans, X-ray, blood tests, iron infusion, blood pressure, ECG, MRSA and Covid swabs and a lengthy consultation. I was told the PET-CT scan was now clear of cancer, which made it all the weirder that I was about to have this huge operation when my body was apparently well.
But here I was, on the promise that this life-changing surgery to remove my sternum could buy me many more years of life. Oncologists had even uttered the word ‘curative,’ which is hard to get your head around when you have incurable breast cancer. Ultimately, they were removing my sternum in the hope that they’d remove all trace of cancer cells for as many years as possible.
The hospital where I had my surgery is not a cancer hospital. The Royal Brompton is a specialist chest hospital, where they do open heart and lung surgeries. I was treated there because I needed a specialist thoracic surgeon to open up my chest, remove my sternum bone and fill the gap with surgical cement. That surgeon and his team were joined by a plastic surgeon from the Royal Marsden, who sliced my latissimus dorsi muscle from my back and placed it over the cement to increase the chance of my body accepting it. As a bonus, he also plumped up my left boob, which had started to look like a bruised peach in the decade since I’d had a smallish tumour removed in 2012.
After my friend dropped me off, I was serenaded by two hipster musicians who were voluntarily delivering a bit of joy to the patients. I felt a fraud lying in my hospital bed, clapping along to their tunes, when I hadn’t yet had my surgery.
Some hours later, I would be serenaded by a new kind of noise: the multi-toned beeps and bleeps of the various drips and machines attached to the other patients by wires. I got zero sleep, and in the morning, my curtain was pulled back to reveal a team of eight or so surgery-ready medical staff.
“Will you ask me to count down from ten?” I said, as I lay back on the bed, an hour later, surrounded by anaesthetists.
“They only do that in the movies,” they said, “but we can, if you like.”
Press for morphine
The next thing I remember is waking up in a recovery room, six hours later, speaking Portuguese to one of the doctors. (This is a very ‘me’ thing to do, showing off my language skills while coming round from a general anaesthetic, desperately trying to prove something.)
They gave me a hand-held contraption with a pain button, which I was instructed to press for morphine as often as I needed. There was no way to overdose; the machine would automatically stop dispensing when it reached its maximum, and I should therefore press it liberally.
“Did you call Mark?” I asked, desperate to know my loved ones had been put out of their misery.
They replied that yes, my next of kin had been told I was awake.
Three hours later, the lead surgeon came into the room and asked how I was doing. I pressed for morphine for the umpteenth time, nodding that I felt better than expected. Then he said: “Shall we call Mark?”
It turned out my next of kin had not been called earlier, and that my parents and Mark had waited from 8am to 6pm to know if my operation had been a success. Dad said it was the longest day of his life.
By the time mum and Mark arrived, I was in a private room in the high-dependency unit, a branch of intensive care where you’re given one-to-one attention from your own dedicated nurse. For my first night, I was cared for by Ajie, the NHS nurse I’ll never forget. He got me through the night, gently tying my hair up and feeding me water with a straw, while taking my bloods and other observations with the maximum care. He was patient, sweet and kind, and I felt like I was in the hands of an angel.
At midnight, I told him my novel, Single Bald Female, was coming out that day in paperback, and I broke down in tears. I'm not sure he even believed me, but he said he couldn't wait to buy it. I woke up a little later, blissed out on morphine, and cried happy tears, telling him what an amazing and important job he was doing and how much I appreciated him. He took my hand and was emotional too, but moments later, he asked me to squeeze his hand to check it was working, because I’d forgotten to squeeze back.
In the morning, Ajie was gone, and I was greeted by a new nurse. I could hear from her accent she was Portuguese, so I asked where she was from, and she told me she was from Matosinhos. I broke into happy tears. Matosinhos was the place where Mark and I got engaged last summer! Everything felt so surreal and serendipitous, like my life was happening exactly as it should.
In that first day post-surgery, I ‘celebrated’ my paperback publication in a haze, but in truth I don’t remember much. Mark and Mum visited supermarkets and book shops to take photos of my novel in the wild, while I focused on trying to breathe and not to vomit.
On the second day in high-dependency, I was cared for by Catarina, my boot camp trainer. She was incredibly kind, but she wasn’t going to let me rest. She knew those first few days were crucial to my recovery, and she was going to make sure I pushed myself as hard as possible. So, despite the fact that I was puking and could barely stomach a drop of water, she pushed me to eat and drink and visit the loo on my own, and take my first steps down the corridor. Catarina was brilliant at her job: the perfect mix of strict and kind.
Much to my disapproval, after two nights in high-dependency, I was moved to a normal ward, where the ratio was one nurse to six patients. It felt like jumping off a cliff, and I didn’t know how I was going to cope without one-on-one care.
Sure enough, it was hard. There were five other women in bay D, each in varying states of repair after operations on their hearts and lungs. Every few minutes, someone’s machine would beep, protesting over an empty bag of morphine or a malfunctioning cannula.
The nurse on shift flitted between our beds, barely managing to keep up with a roster of tasks that included taking our heart rates and blood pressure, administering upwards of 40 different pills per person, emptying catheters and commodes, and asking the all-important question: “How would you rate your pain on a scale of 1 to 10, where 10 is the worst pain imaginable?”
I was usually a five or six, a score greatly aided by a cocktail of morphine, codeine, paracetamol and an epidural. In those first few days, my main problem wasn’t pain, but a combination of drowsiness, sickness, thirst and constipation. I was made to stay awake against my will, to sit up in a chair to encourage my lungs to regain proper function, to be carted off for x-rays and blood tests when all my body wanted was to sleep. It felt like that TV show, Shattered, where the contestants were made to stay awake for as many days as possible to win the £100,000 cash prize. In other words, torture.
Then there was the sickness. I knew I needed to eat, but the drugs and anaesthesia made me so nauseous I couldn’t stomach a thing. I was so thirsty, my mouth so dry I could barely talk, but I couldn’t manage more than a sip at a time. I asked Mark to bring me some Starburst, but they tasted of syrup and didn’t quench my thirst at all.
In ordinary life, I boast about my brilliant appetite and I even run a podcast about food, but the first few days in hospital, all food made me feel violently ill. When forced to choose from the extensive hospital menu, I would pick the jacket potato or the tuna sandwich, but I’d only manage a few bites before giving up. Mum and Mark brought the foods I craved – fresh blueberries, raspberries and ginger beer to quench my thirst – but I would only vomit them up.
A slew of doctors and nurses arrived by the hour, sometimes announcing their names and titles, sometimes expecting me to know who they were, even behind their masks. They would inspect my scars, ask me to describe my pain and sometimes ask me to choose between unpronounceable anti-sickness medications that I had no idea about.
More often than not, they were kind, patient and gentle, and had time for my questions. But, occasionally, they couldn't quite read the room. One time, a doctor arrived as I was holding a sick bowl and proceeded to inspect my wounds while I painfully puked into the cardboard bowl. Why she couldn’t have waited two minutes to afford me a little dignity, I don’t know.
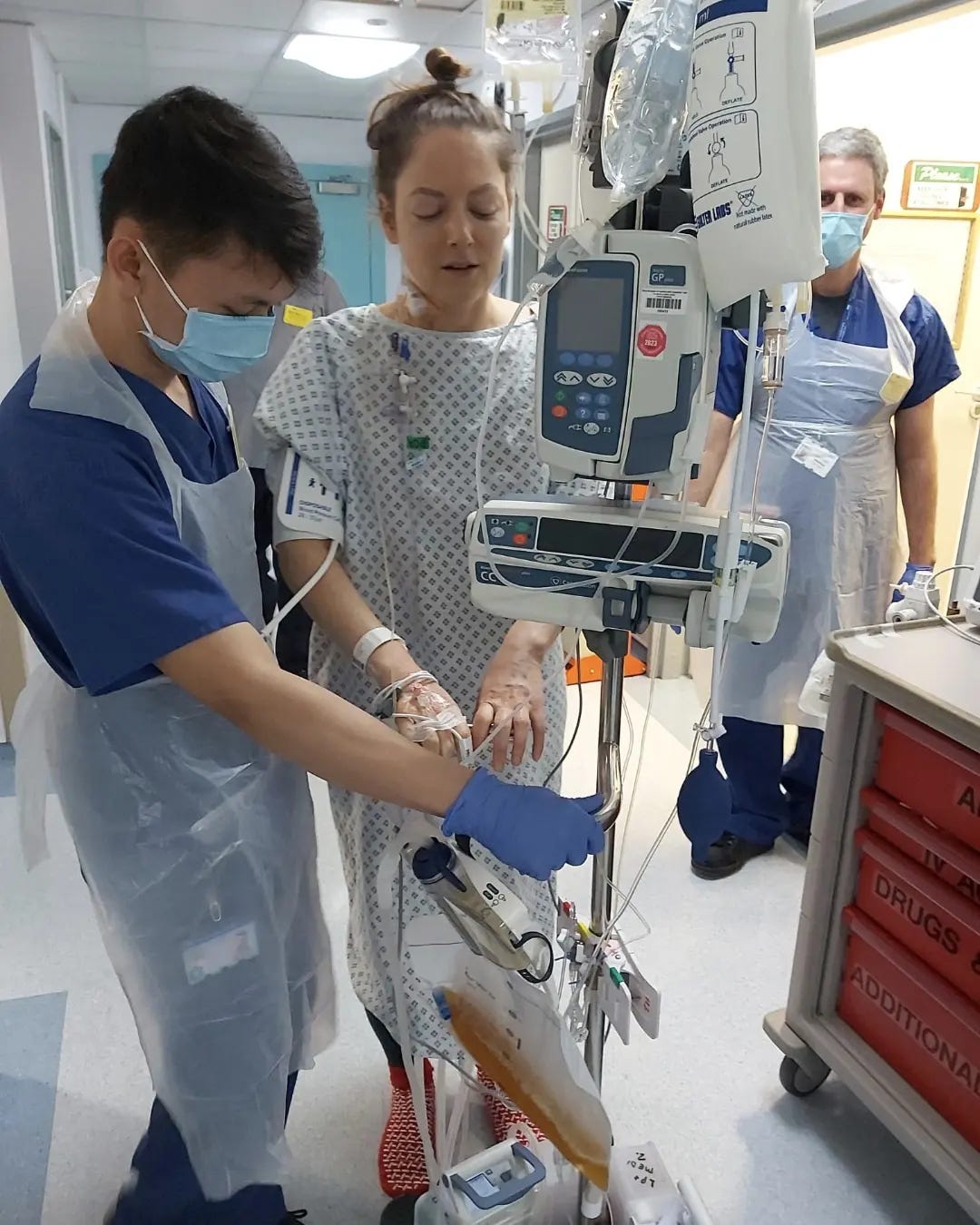
In the first few days, my body wasn’t my own. There were tubes coming out of me at every angle, including my nose, my hand and my abdomen. They’d attached a ‘central line’ cannula in my neck, with several lines off it where they took blood and injected morphine and anti-sickness drugs. A cannula in my hand meant it was difficult to text on my phone, so I left breathless voice notes with updates for my friends.
A catheter collected urine in the first 24 hours before I was able to get to the loo, and four drains collected blood and other fluids from my wound sites. These drains connected to what looked like large multi-compartment Tupperware suitcases, each with its own screen showing how much fluid was being collected. The goal was to get below 100ml per day before the drains could be removed.
It was Catarina who removed the two larger drains, and this five-minute procedure forms one of my more vivid memories. She told me to take three deep breaths in and out, and on the third, I must hold my breath while she and a colleague pulled out the drain. If I didn’t hold my breath properly, air could enter my lungs, and this would be Very Bad Indeed.
I can’t tell you how terrifying it is receiving an instruction like this, where you know you can screw up your own recovery, but you can’t breathe well enough to ensure you’ll do it properly. But Catarina walked me through it, and together we did it. It hurt, but it was momentary. She applied large stitches that looked like unfurled metal paperclips sticking out below my breasts.
By the time I was moved to the women’s ward, I had just two smaller drains attached, plus the cannulas in my neck and hand, and a drip attached to the morphine button. When I wanted to go to the loo, someone had to pick up the suitcase full of my bodily fluids and place it on the base of my drip pole. Then, like a game of reverse Cat’s Cradle, they must untangle the various wires attached to my body so that I could walk, slowly, to the loo, with the drip pole in tow. This alone is enough to make you want to drink very little water, even though you’re completely dehydrated.
Welcome to Phlegm Island
When I moved from high dependency to bay D, everything changed. There were six of us now, and it quickly became clear we were a team. Each woman’s bed had its own blue curtain that could be pulled around it, but the curtain hid none of the moans, groans, farts and bleeps that came from behind it. When one of us pressed the call button or cried out in pain, another would summon the nurse as quickly as possible.
You’ll have to bear with me now, but I couldn’t help comparing it to Love Island. Here we were: six women with extensive bodily modifications (albeit a different kind of plastic surgery) sharing a bedroom and building bonds of friendship. We weren’t coupling up in the romantic sense, but we were working towards a common goal to get out of there as fast as possible.
We came up with the name Phlegm Island largely on account of the fact that these heart and lung patients had been asked to cough as much as possible to make sure the lungs were cleared and working well. (On the first day, I coughed up what looked like an actual piece of bubblegum.)
Every morning, we were woken at the crack of dawn, not by Maya Jama asking us to report to the fire pit, but by a nurse enquiring about the status of our bowel movements. (Constipation was a key part of post-surgery life and formed the basis of approximately 96% of all conversations.)
When anyone was lucky enough to be discharged, we would gather around their bed, fussing and helping them to pack before tearfully wishing them on their way. We would feel a collective nervousness about the newbie who was to fill their bed, but within hours said newbie would be welcomed into the fold as if they’d been there forever.
Most of the patients were at least 20 years my senior, but this didn't matter. My closest friendship developed with a woman named Jennie, who was a little younger than my mum. One day, after I mentioned the hospital mugs were remarkably heavy for patients with massive chest trauma, my new friend sent her partner out to buy me a mug. It was the simplest act of kindness, but it felt like everything in there.
As the six of us started to get better, we spent less time lying horizontal and more time chatting. My appetite was slowly returning, and one day I sat on the end of my bed and said: “What’s the first thing you’re going to eat when you get out of here?”
The question was met with a collective “Ooooh!”. Everyone was so excited about what they would eat when they got into the Outside World. We had started to visualise ourselves getting back into society, doing things that constituted Normal Life. It’s funny that we felt that way after just a week or so, but it’s hard to imagine things carrying on as normal when you’re so absorbed in hospital life.
Within days, I came to learn which of my campmates had had their first poo, a real milestone in the process. When we trundled towards the loo with our drip poles in tow, there would be collective calls of ‘good luck.’ Our return might be met with a thumbs up, or a voluntary report on whether we’d finally managed a number two. (Spoiler alert: I never had.)
I’ve mentioned my nausea, but I only ever vomited small amounts of liquid. This meant that every meal I ate stayed inside me, until at some point my body contained nine days’ worth of jacket potatoes and tuna sandwiches. I can’t tell you how much it hurts when your belly is swollen and puffed up like a whale’s, and there’s no relief in sight.
After a week of consuming all the laxatives under the sun, we tried a suppository, where a nurse inserts a tablet-type thing up your bum. I’m sure you’ll be mortified to hear about this, but there’s no room for embarrassment when you’ve had nearly 11 years of this stuff.
When the suppository didn’t work, we tried an enema, which is where they squirt some liquid up with a syringe. This is by no means the official explanation, but I imagine it works like that industrial-strength sink unblocker, with chemicals breaking down the Fatberg in your intestines.
Sadly, 3,000 laxatives, one suppository and two enemas offered little relief, so eventually I gave up and waited for nature to take its course.
And on day 10, she opened her bowels
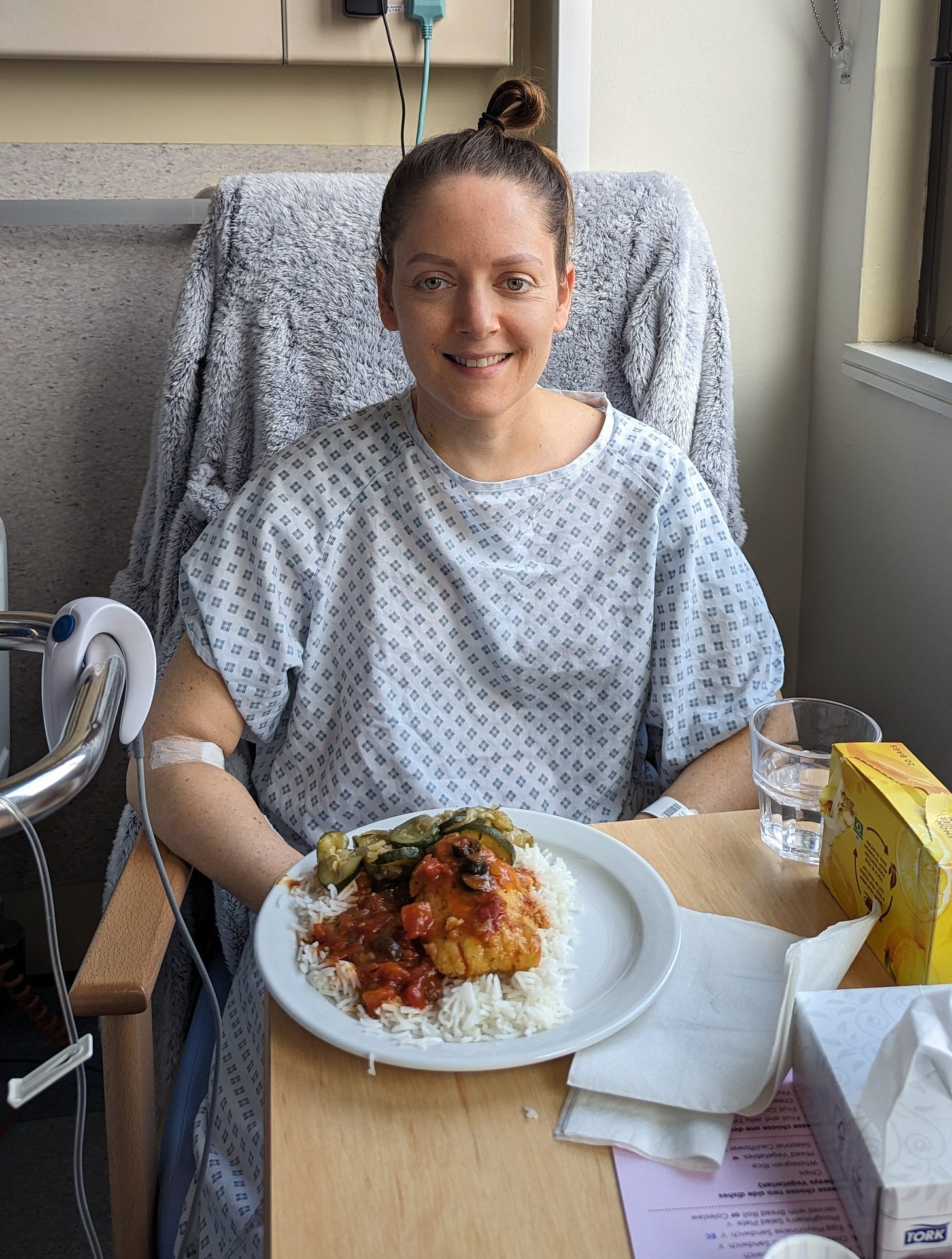
It’s about time I mention that the hospital food was DELICIOUS. As the sickness abated and my appetite increased, I looked forward to picking my order from the daily menu, and I scarfed down curries and soups with gusto. We measured my recovery by my appetite, and Mark took great pleasure from every spoonful of yoghurt or jacket potato he managed to feed me.
Visitors like Mark and my mum were vital. There was only one nurse for six patients, and that nurse was run off their feet for their entire 12-hour shift. If you wanted a cup of tea outside of mealtimes, you could only get it if you had a visitor. Sure, a nurse could tie up your hair if you were desperate, but you could only ask so much.
All of the nurses were wonderfully patient and kind, despite being so busy. But occasionally, you’d get the sense you were asking too much, and you’d find yourself apologising while asking for that lidocaine patch or morphine refill.
One day, perhaps due to confusion after the staff handover, the team let both my epidural and my morphine completely wear off. It was several hours in before I realised what had happened, and by that point I was in significant pain. When the pain meds finally set in again, I lay back in bed and hallucinated jungle creatures. It was a surreal yet not unpleasant experience and one that was not uncommon among my campmates.
Despite its first-rate expertise and care, the hospital was weirdly ill-equipped for patients recovering from chest trauma. Sink taps were too heavy to turn on, paper towel dispensers were placed inaccessibly high, milk was supplied in two-litre bottles no patient post-lung-surgery could ever lift, and shower rooms lacked shelves so you’d have to slut-drop for your shampoo. If you didn’t have a visitor, you would really struggle.
I hated feeling so dependent on others. Mark and my mum were amazing, bringing me everything I craved and pandering to my every whim. But they were both sacrificing so much – Mark was in a state of shock and grief over his father’s death while juggling hospital trips with his job and children, while mum was travelling the literal length of the country visiting me and other sick relatives.
Yet they were so vital to my recovery. On the eighth day, when all my tubes were removed and I was finally able to take a shower, Mum took me in and helped me wash. Until that moment, I’d usually dressed or undressed with my back turned, but now she was seeing my body, hunched from the surgery and covered in scars and dressings. It can’t have been easy seeing me that way.
Meanwhile, when I was in a haze of complete nausea, pain and drowsiness, with a rock-hard bloated belly, Mark looked at me and told me he'd never seen me looking so beautiful. (I know he meant it, although trust me, I've never looked so shite.)
The final straight
As time went on, one by one, the original six women were well enough to be discharged, and it was just Jennie and me left.
“We’ve reached the Phlegm Island final!” I said to her, laughing.
We had crossed so many milestones together – getting dressed for the first time, having our drips and tubes removed, the first shower. We’d been through such a lot from the first night to the last, and it felt surreal to be nearing the final straight together.
My novel, Single Bald Female, is about two friends who meet in a cancer hospital. While parts of the book were inspired by my own experiences, the friendship storyline is entirely fictional. And now, suddenly, I felt like I was living my own book. I’d made that special friendship that only comes from the most challenging of times, and it really made the whole experience worth it.
In the end, Jennie was discharged a few hours before me, which technically made me the Phlegm Island winner. But we both got to go home, we both gained a friend, we both made memories that will last a lifetime. I’m pretty sure it was a joint victory.
As for Ajie, the nurse who cared for me that first night in high dependency, I found him in the corridor on my last day, and gave him a signed copy of my book. It wasn’t much in return for his wonderful care, but he was happy and grateful, and we both got a little emotional.
Ajie is one of many, many angels in the NHS. The work they do is the most important work there is. We need to pay them more, give them better conditions, treat them with kindness, always. I will forever be grateful to everyone who treated me at the Royal Brompton – the amazing surgeons, the wonderful nurses, the catering staff, the porters and the cleaners. I know the NHS is in crisis, but we are truly, truly fortunate to have such an incredible health service at our disposal in the UK. We must do everything in our power not to let it break.
Three books and one podcast to consume after this
I’m conscious that millions of people spend much more time in hospital with much more serious conditions than mine, and that the experience I’ve shared here is mine and mine alone. Here are some other things I recommend:
— We All Want Impossible Things by Catherine Newman is a novel about the friendship between two women, one who is dying in a hospice and the other who is by her side. It’s so perfect in describing the hospice experience, and so much of it reminded me of my hospital experience. I fear my 2023 reading may have peaked.
— Driving Forwards by Sophie L. Morgan. Sophie was paralysed in a car crash when she was 18, but she’s built the most incredible life as a TV presenter. Her audiobook is completely brilliant, and it’s out now in paperback too.
— Single Bald Female by me. Yes, I’ve mentioned it a few times! It’s about two friends who meet in a cancer hospital and it’s never felt more relevant. You can currently buy it in paperback for as little as £4 (!) and it’s in Tesco, Asda, book shops and online. Please do buy it and review it, to help enable me to write more books in future.
I also interviewed the incredible former palliative care doctor, Dr Kathryn Mannix, about Food and Death for my podcast, Life in Food. We spoke about some of the cultural experiences that exist around food and funerals, as well as the concept of a Death Café, and lots of talk of cake. Listen here.
I’ll update you soon with how my recovery is going (spoiler alert: I still have stage four cancer), but in the meantime if you’re not already following me on Instagram or Facebook then please do, as there are more updates there.
Thanks for reading, and please do subscribe and share this newsletter!







As always Laura you are totally inspirational! I'm so glad you have made it through the operation and out the other side, albeit with more mountains to climb I'm sure! You are an amazing girl! I am in total awe and it's a privilege to read your email. Love and hugs you and yours xx
Estou disponível para conversas em português com sotaque brasileiro. 🤗